A Breakthrough in Aortic Root Treatment
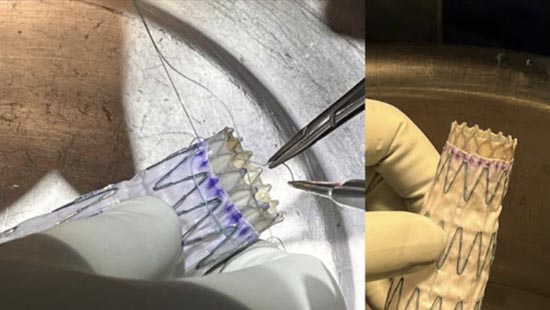
Hand-sewn self-expanding TAVR valve inside tapered TEVAR graft, courtesy of the American Heart Association.
The innovators on the aortic team at the University of Maryland Medical Center (UMMC) have now twice effectively repaired acute type A aortic dissection (ATAAD) involving aortic root via a complete endovascular replacement known as the Endo-Bentall procedure. This pioneering procedure seems to be the first-ever successful combination of a self-expanding transcatheter aortic valve (TAVR), a tapered endovascular stent graft (TEVAR) and wire-reinforced fenestrations for coronary artery stenting to treat ATAAD in a minimally invasive manner.
The team, co-led by Shahab Toursavadkohi, MD, Associate Professor of Vascular Surgery at UMSOM and Co-Director of the Center for Aortic Disease, is advancing medicine and recreating the approach to treating ATAAD. Until now, there have been no commercially available endovascular devices designed for aortic root repair, but with this physician-constructed Endo-Bentall device, the need for cardiopulmonary bypass (CPB) is eliminated, offering a viable option for high-risk patients who are otherwise unsuitable candidates for the open Bentall procedure.
Crafting the Graft
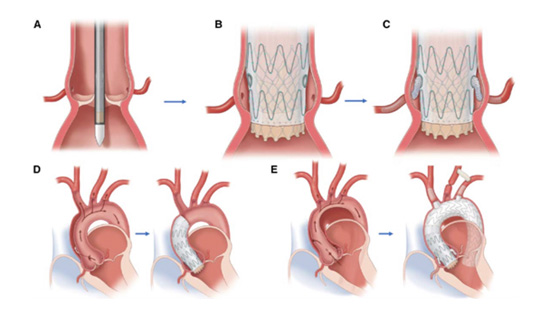
An illustration of the Endo-Bentall repair device inside the aorta, courtesy of the American Heart Association.
The novel Endo-Bentall device is a modified composite graft created from conjoining a TEVAR stent graft and a self-expanding TAVR valve currently available on the market. Wire-reinforced fenestrations are created with segments of nitinol guidewire in the graft to allow adequate perfusion of the coronary sinuses and provide access for any subsequent coronary artery stenting that may be necessary after deployment. These fenestrations were reinforced with radiopaque nitinol wires so they could be accessed in the future if needed. The TAVR valve is circumferentially sutured to the TEVAR graft and subsequently re-sheathed within the TEVAR delivery system and flushed with C02 and rifampin.
Patient Population
This procedure was designed for patients with ATAAD with aortic root involvement or with any other aortic root syndromes who, for various reasons, are deemed too high-risk for an open Bentall operation. The first case was a 63-year-old female with stage IV metastatic endometrial cancer and ATAAD with a primary-entry tear in the noncoronary cusp and severe AI. She was deemed a nonsurgical candidate due to her ongoing chemotherapy and immunotherapy treatments. The second case was an 85-year-old female with a 6.3 cm ascending aortic aneurysm, acute on chronic ATAAD originating in the sino-tubular junction and aneurysmal dilation extending into the aortic root, ascending aorta and aortic arch. Given her advanced age and poor functional status, this patient was also not a surgical candidate.
Procedure
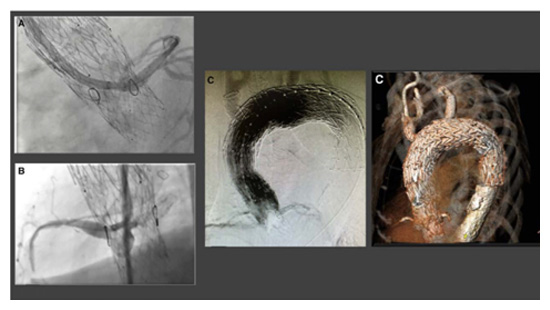
The Endo-Bentall device, which was deployed in a patient by University of Maryland Medical Center's aortic team, image courtesy of the American Heart Association.
This operation is performed with the collaboration of three teams simultaneously, including cardiac surgery, vascular surgery, and interventional cardiology. One team prepares the device while the other team obtains vascular access. For this technique, groin arteries are accessed percutaneously and no major incision is required. The modular device is advanced via femoral access and is positioned in the aortic root. After confirmation of the appropriate location of the device, the graft is deployed under rapid pacing of the heart. If endoleak presents after graft deployment, coronary stenting is performed.
Outcomes
There were no immediate complications for either of the patients. In the first case, the patient was discharged from the hospital post-op day 16 and resumed chemotherapy and immunotherapy shortly after discharge. This patient expired five months post-op after developing severe urosepsis. The second case involved an 85-year-old female with an aortic aneurysm and aortic dissection. The patient was discharged from the hospital a week later without any complications. A three-month follow-up CTA demonstrated complete false lumen thrombosis.
Conclusion
Further testing and follow-up are needed to evaluate these physician-modified devices' long-term durability and reproducibility. Endo-Bentall is a realistic option for patients with aortic root syndromes who are too high risk for conventional open surgical repair.
The preoperative planning and execution of this procedure involved a collaborative effort from the multidisciplinary team at UMMC. Composed of cardio-aortic surgeons, heart valve structure surgeons, interventional cardiologists, vascular surgeons, and other medical professionals, this groundbreaking procedure showcases an innovative endovascular approach to treating complex aortic disease.
“The Endo-Bentall is a groundbreaking step forward in aortic root/ascending aortic repair and means that more people can survive these devastating Type A dissections in a less invasive manner,” says Bradley S. Taylor, MD, MPH, the Dr. Joseph S. and Irene P. McLaughlin Professorship in Cardiothoracic Surgery, Professor of Surgery, and Chief of Cardiac Surgery at UMSOM. “This kind of innovation is a testament to the incredible teamwork and collaboration we are fortunate to enjoy here at the University of Maryland Medical Center.”
References
Ghoreishi, M., Chahal, D., Shah, A., Hirsch, J., Tran, D., McCloskey, D., Shkullaku, M., Gupta, A., Strauss, E. R., Dahi, S., Kang, J., Taylor, B. S., & Toursavadkohi, S. (2023). First-in-Human Endovascular Aortic Root Repair (Endo-Bentall) for Acute Type A Dissection. Circulation: Cardiovascular Interventions.
