History | University of Maryland Neurosurgery
The Beginnings of Medical Education in Neurosurgery

1807
The College of Medicine of Maryland, eventually the University of Maryland School of Medicine, was established, the first public medical school and the fifth medical school in the country.
1920
The Society of Neurological Surgeons was formed with the interest of 11 surgeons, including Dr. Charles Bagley Jr.
Neurosurgical Training Emerges at University of Maryland

Dr. Charles Bagley
1930
Charles Bagley Jr. became Professor and Head of the Section of Neurological Surgery at the University of Maryland, where he implemented the residency program. In 1913 he was Dr. Harvey Cushing’s last neurosurgery resident at Johns Hopkins Hospital and first neurosurgery resident at the Peter Bent Brigham Hospital.
During World War I, Dr. Bagley served in the neurosurgical section of the Office of the Surgeon General in Washington and later in France. In 1931 he served as the President of the Society of Neurological Surgeons. At the University of Maryland he made progress in the science of head trauma and neurosurgery.
He delineated the significance of blood in cerebrospinal fluid. Dr. Bagley trained a generation of neurosurgeons.
1939
William B. Scoville, after training at MGH, spent 6 months learning prefrontal lobe surgery at the University of Maryland. He started his practice in Hartford, Connecticut. He is known for later performing bilateral medial temporal lobectomies on patient H.M. to alleviate epilepsy, who unfortunately suffered anterograde amnesia. This case significantly influenced modern memory science and neuroscience.

Left: A schematic of the “pallidotomy surgical instrument” developed by Dr. William W. McKinney and machinists Robert A. Hasty and Leslie S. Noska (Patent US3055370A)
Right: A schematic of the automatic craniotomy drill developed by Dr. George W. Smith (Patient US002842131)
1941
William W. McKinney was the first neurosurgery resident to graduate from the University of Maryland.
He was from Texas and continued his practice there, becoming the first neurosurgeon in Fort Worth.
He is known for his early work in performing cerebral angiograms for the diagnosis of brain tumors.
He developed the McKinney Pallidotomy Guide, patented in 1958, and the McKinney Stereotactic Frame, which were used to treat patients with Parkinson’s disease.
Watch this video about William W. McKinney.
1944-1950
George W. Smith developed the automatic craniotomy drill while training and then working with Dr. Bagley, which he patented in 1958. His design and its derivations are in wide use today.
He also developed the vessel-encircling aneurysm clip and introduced the modern technique for anterior cervical discectomy and fusion. Dr. Smith later founded the neurosurgery residency program at the Medical College of Georgia.

First row: James G. Arnold, Charles Bagley Jr, Robert M. N. Crosby, Raymond K. Thompson, Frank Otenasek, George W. Smith (1952)
1947-1993
Raymond K. Thompson graduated (‘47) under the tutelage of Dr. Bagley. He made contributions to the pathological anatomy of brainstem trauma. He served as a lieutenant in the United States Naval Reserves during World War II. Dr. Thompson also served as President of the Congress of Neurological Surgeons in 1958.
Along with Dr. Mosberg, he was one of the founders of the Foundation for International Education in Neurological Surgery. He was a neurosurgeon at the University of Maryland for his entire career. Dr. Thompson was a source of stewardship and constancy.
1951
Robert M. N. Crosby graduated from the neurosurgery program. Dr. Crosby was one the first neurosurgeons to practice almost exclusively in pediatrics. His seminal work, The Waysiders, explained dyslexia as a neurological disorder, decreasing its social stigma. Dr. Crosby not only served Baltimore as a pediatric neurosurgeon, he was also a national advocate for children. He served as Chairman of the National Advisory Committee on the Education of the Handicapped under President Nixon. Dr. Crosby was a founding member of the Pediatric Neurosurgery Division of the AANS.

Early focused ultrasound system developed by Fry, Mosberg, Barnard, and Fry. Depicted are four ultrasound elements converging on a focal point to allow for targeted ablation. Modern focused ultrasound systems use more than 1,000 elements (JNS. 1954:11(5):471-8)
1952-1954
University of Maryland neurosurgeon William H. Mosberg Jr. (‘49) worked with the Fry brothers to develop focused ultrasound ablation of the brain. They reported the advantages of this technology, including “no disturbance to brain tissue except in the focal region.”
With Dr. Thompson, Dr. Mosberg was one of the early founders of the Foundation for International Education in Neurological Surgery, an organization that provides and bolsters neurosurgical education in developing countries. He served as President of the Congress of Neurological Surgeons in 1966.
In 1992, he received the Humanitarian Award from the AANS.
1952-1984
James G. Arnold became Chair of Neurosurgery in 1952. He led the program for decades. Dr. Bagley and Dr. Hugh R. Spencer, Chair of Pathology, started one of the country’s first neuropathology laboratories. Dr. Arnold contributed significantly to this effort. The Resident Library is named after Dr. Arnold.
Dr. Bellegarrigue (‘80) treating a patient in the neurosurgical intensive care unit at Shock Trauma, featured in the Baltimore Sun Magazine (1977)
1958
The country’s first clinical shock trauma center was established by the efforts of Dr. R. Adams Cowley, and a grant from the U.S. Army.
The Shock Trauma Center became the first and only integrated trauma hospital.
In 1980, Jon Franklin and Alan Doelp published Shock-Trauma, an account of the challenges faced in this unique environment.
Guidelines and practices developed at Shock Trauma have become the national standard of care.
1975-1976
Thomas Barbee Ducker served as Chair of Neurosurgery. His and Dr. Salcman’s harrowing efforts to treat a patient suffering from a brainstem arteriovenous malformation with two aneurysms was recounted by Jon Franklin for the Baltimore Sun, which won the inaugural Pulitzer Prize in Feature Writing in 1979, titled “Mrs. Kelly’s Monster,” becoming a milestone in immersion journalism.
1983
David W. Cahill finished his training in neurosurgery at the University of Maryland. Dr. Cahill was an internationally recognized expert in complex spine surgery. He started the Department of Neurosurgery at the University of South Florida, and its residency program. After his untimely death, a robust forum to discuss controversies in spine surgery was named after him, commemorating his lively spirit, the Cahill Session at the AANS/CNS Annual Meeting of the Spine and Peripheral Nerves.
1984
Michael Salcman becomes Chair of Neurosurgery. He investigated the use of microwave implants for the disruption of the blood brain barrier and the treatment of brain tumors. He served as President of the Congress of Neurological Surgeons in 1991. Dr. Salcman is an acclaimed author and poet and continues to practice and teach his craft.
Modern-Day Department of Neurosurgery
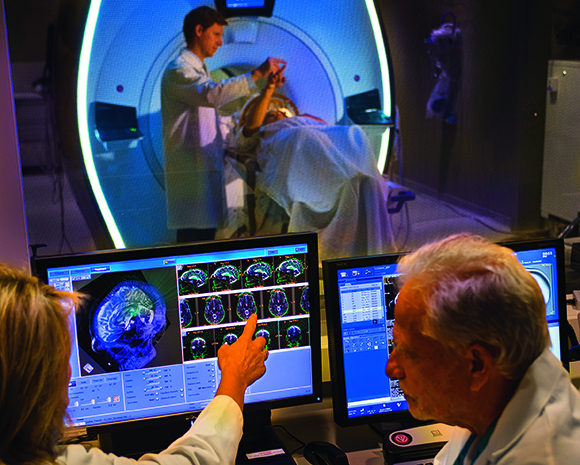
Howard Eisenberg, MD, right, and Graeme Woodworth, MD, treating a patient with essential tremor using focused ultrasound.
1991
Howard M. Eisenberg became the R.K. Thompson Chair of Neurosurgery and the Department of Neurosurgery was established.
In 2000, he served as the President of the Society of Neurological Surgeons. Dr. Eisenberg was a founding member of the American Society of Pediatric Neurosurgery.
Over his long career, he has made significant contributions to the understanding of hydrocephalus, brain and spinal cord trauma, and more recently, the treatment of movement disorders with magnetic resonance-guided focused ultrasound surgery.
1992
Gamma Knife Radiosurgery was integrated into neurosurgical care for brain tumors, nerve compression syndromes, and arteriovenous malformations.
2001
The Simard Laboratory discovered the novel SUR1-TRPM4 channel and described its role in cerebral edema. These discoveries lead to ongoing clinical trials testing the use of SUR1 inhibitors for the treatment of cerebral edema after acute CNS injury.
2012
Continuing the University of Maryland’s history with focused ultrasound surgery, the magnetic resonance-guided focused ultrasound program was established. Treatment began for patients with essential tremor.
2018
The Department of Neurosurgery continues to treat patients with essential tremor weekly using focused ultrasound. The first patients in the country received focused ultrasound treatment for Parkinson's disease and for neuropathic pain. The first patient in the country with a brain tumor was treated with focused ultrasound for blood brain barrier disruption.
2019
Graeme Woodworth, MD was selected to succeed Dr. Eisenberg as Department Chair.
Dr. Woodworth came to the University of Maryland to expand and enhance the neuro-oncology program including new research focuses on nanomedicine and focused ultrasound.
His team treated the first brain tumor patient in the United States with MRI-guided transcranial focused ultrasound for blood brain barrier disruption, continuing the long-standing Maryland tradition of neurosurgical innovation and advancement of this promising technology.


