A Patient's Guide to Lumbar Herniated Disc
Lower back problems can occur for many different reasons. The terms ruptured disc and slipped disc seem to be used more commonly in the last few decades. People often assume that everyone who has back pain has a ruptured disc. However, a true herniated nucleus pulposus (the official medical name for this problem) is not very common. Most problems that cause pain in the back are not due to a herniated disc.
For a more in-depth discussion of the parts of the spine and how they work, along with a general overview of back and neck problems, you might want to review the document, entitled:
Let's look at what a herniated disc really is, how it causes problems, and how the condition is diagnosed and treated by a back specialist.
Anatomy
To better understand how a herniated disc occurs, it is helpful to know some anatomy of the spine and more specifically, the parts of the spine involved
Please review the document entitled:
The intervertebral discs are the cushions that act as shock absorbers between each of the vertebra in your spine. There is one disc between each vertebra. Each disc has a strong outer ring of fibers called the annulus, and a soft, jelly-like center called the nucleus pulposus.
The annulus is the disc's outer layer and the strongest area of the disc. The annulus is actually a strong ligament that connects each vertebra together. The mushy nucleus of the disc serves as the main shock absorber.
A herniated disc occurs when the intervertebral disc's outer fibers (the annulus) are damaged and the soft inner material of the nucleus pulposus ruptures out of its normal space. If the annulus tears near the spinal canal, the nucleus pulposus material can push into the spinal canal.
Causes
Herniated discs can occur in children, although this is rare. Usually a true herniated nucleus pulposus is most common in young and middle-aged adults. In older folks, the degenerative changes that occur in the spine with aging actually make it less likely for them to develop a true herniated disc.
Discs can rupture suddenly because of too much pressure all at once on a disc. For example, falling from a ladder and landing in a sitting position can cause a great amount of force across the spine. If the force is strong enough, either a vertebra can fracture or break, or a disc can rupture. Bending over places a great amount of force on the discs between each vertebra. If you bend and try to lift something that is too heavy, the force can cause a disc to rupture.
Discs can also rupture from a small amount of force - usually due to weakening of the annulus fibers of the disc from repeated injuries that add up over time. As the annulus weakens, at some point you may lift something or bend in such a way that you cause too much pressure across the disc. The weakened disc ruptures while you are doing something that five years earlier would not have caused a problem. Such is the aging process of the spine.
A herniated disc causes problems in two ways. First, the material that has ruptured into the spinal canal from the nucleus pulposus can cause pressure on the nerves in the spinal canal. There is also some evidence that the nucleus pulposus material causes a chemical irritation of the nerve roots. Both the pressure on the nerve root and the chemical irritation can lead to problems with how the nerve root works. The combination of the two can cause pain, weakness, and/or numbness in the area of the body that the nerve usually goes.
Symptoms
The symptoms of a true herniated disc may not include back pain at all! The symptoms of a herniated disc come from pressure on, and irritation of, the nerves. However, many people do have back pain because they have other problems in their back when the disc ruptures. The symptoms of a herniated disc usually include:
- Pain that travels into one or both legs
- Numbness or tingling in areas of one or both legs
- Muscle weakness in certain muscles of one or both legs
- Loss of the reflexes in one or both legs
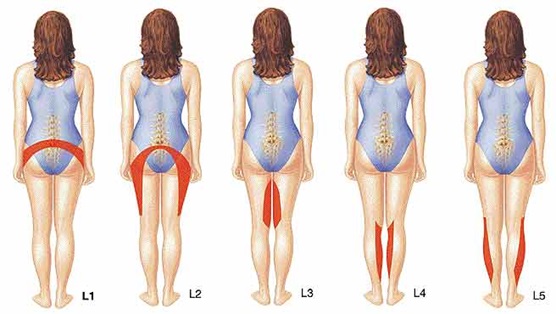
Where these symptoms occur depends on which nerve(s) has been affected in the lumbar spine. Therefore, the location of the symptoms helps determine your diagnosis. Knowing where the pain is perceived gives your doctor a better idea of which disc has probably ruptured.
Diagnosis
Making the diagnosis of a herniated nucleus pulposus begins with a complete history of the problem and a physical examination. The main questions your doctor will be interested in are:
- Did you have an injury?
- Where is the pain?
- Do you have any numbness? Where?
- Do you have any weakness? Where?
- Have you had this problem or something like it before?
- Have you had any weight loss, fevers, or illnesses recently?
Finally, your doctor will be interested in knowing if you have problems when you have to urinate or have a bowel movement. This is important to make sure there is no pressure from the herniated disc on the nerves that go to the bowels and bladder. If you do, this may be an emergency, and require immediate surgery.
Your doctor may suggest taking X-rays of your lower back. Regular X-rays will not show a herniated disc, but they will give your doctor an idea of how much wear and tear is present in the spine and may show other causes of your problem.
The most common test done today to diagnose a herniated disc is the MRI scan. This test is painless and very accurate. As far as we know, it does not have any side effects. It has almost completely replaced other tests, such as the myelogram and CAT scan, as the best test to do (after X-rays) if a herniated disc is suspected.
Sometimes, the MRI does not tell the whole story. Therefore, other tests may be suggested. A myelogram, usually combined with a CAT scan, may be necessary to give as much information as possible. Still, if it has not been confirmed that the pain is coming from a herniated disc, additional, more specialized tests may be conducted. Electrical tests (such as the EMG and SSP) can confirm that the pain in your leg is actually coming from a damaged nerve. These tests may be required before a decision is made to proceed with surgery.
Treatment
Just because a disc has herniated does not necessarily mean that you will need to undergo surgery. In the majority of cases, a herniated disc will probably not require surgery. Treatment of a herniated disc depends on the symptoms. It also depends on whether the symptoms are getting steadily worse - or whether they are getting better. If the symptoms are getting steadily worse, your doctor may be more likely to suggest surgery. If the symptoms are getting better, he may suggest watching and waiting to see if the symptoms go away. Many people, who initially have problems due to a herniated disc, find that they completely resolve over several weeks or months.
Conservative Treatment
Observation
You may not need any treatment other than watching to make sure that the problem does not progress. If the pain is bearable and there is no progression of weakness or numbness, your doctor may just suggest watching and waiting.
Rest
If the pain is more severe, you may need to take a few days off from work and decrease your activity for a while. After several days, you should begin to mobilize yourself. Begin a gentle walking program and increase the distance you walk each day.
Pain Medications
Depending on the severity of your pain, different approaches can be used to help control your pain with medications. Over-the-counter pain relievers, such as ibuprofen, Tylenol, and some of the newer anti-inflammatory medications may help reduce your pain. Make sure you follow the directions and do not take too many. If these types of medications do not control your pain, your doctor may prescribe stronger pain pills - narcotic or non-narcotic pain medications. Narcotic pain medications are very strong, but also very addictive. Non-narcotic pain medications are less addictive, but are somewhat less effective than the narcotics. Most physicians do not like to prescribe narcotics for more than a few days or weeks!
Epidural Steroid Injection (ESI)
The ESI is usually reserved for more severe pain due to a herniated disc. It is not usually suggested unless surgery is fast becoming an option to try to reduce your pain. The ESI is probably only successful in reducing the pain from a herniated disc in about half the cases that it is used.
Surgical Treatment
Laminotomy and Discectomy
The traditional way of treating the herniated disc with surgery is to perform a laminotomy and discectomy. The term laminotomy means "make an opening in the lamina", and the term discectomy means "remove the disc".
This procedure is performed through an incision down the center of the back over the area of the herniated disc. Once the incision is made through the skin, the muscles are moved to the side so that the surgeon can see the back of the vertebrae. X-rays during surgery may be required to make sure that the correct vertebra is chosen. A small opening is made between the two vertebrae where the disc is ruptured. This allows the surgeon to see into the spinal canal. The term laminotomy (make an opening in the lamina) comes from the fact that usually a small amount of the bone of the lamina must be removed. This is to make room to see into the spinal canal and to allow room to work.
Once this is done, the surgeon moves the nerve roots out of the way to see the intervertebral disc. The surgeon locates the disc material that has ruptured into the spinal canal and removes it. This removes any pressure and irritation on the nerves of the spine. Using small instruments that fit inside the disc itself, he also removes as much of the nucleus pulposus material still inside the disc as possible. This is done to prevent any remaining disc material to herniate again after the operation.
After the procedure is complete, the muscles of the back are returned to their normal position around the spine. The skin incision is repaired with sutures or metal staples.
Microdiscectomy
Recently, improvements have been made in the tools available to the spinal surgeon for performing a laminotomy and discectomy. The procedure is essentially the same as the traditional way of removing a ruptured disc; however, it requires a much smaller incision. The advantage of this procedure over the traditional approach is that there is less damage to the normal parts of the spine during the operation. You may also recover faster.
To be able to see through the smaller incision, the surgeon uses an operating microscope. A small incision (as small as two inches) is made in the back just above the area where the disc is herniated. Once the muscles are moved aside and the vertebra can be seen, a microscope is used to finish the operation. The rest of the operation is performed exactly like the more traditional approach described above.
Endoscopic Discectomy
Many surgical procedures have been revolutionized by the use of special TV cameras. The procedure is still the same, but even smaller incisions (1/4 inch) are made to insert a special magnified TV camera into the spinal canal so that the surgeon can actually see the disc material. Through these small incisions, the camera and several other surgical instruments are inserted. Rather than look through a microscope, he watches the TV screen while he directs the specially designed instruments to remove the disc material.
Torn cartilages of the knee are now routinely removed with the arthroscope, and gallbladders are routinely removed with the laproscope. The same approach is evolving with spine surgery. The notion is that if microdiscectomy can do less damage because of a smaller incision, endoscopic discectomy could do even less damage. This surgical procedure is still evolving and is not yet widely used.
This procedure has the benefit that it does even less damage to the normal tissues around the spine during the operation. This can lead to a still faster recovery and less complications.
Complications
Please review the document, entitled:
Before Surgery
Even before surgery, there can be complications of a herniated disc. The most serious complication from a herniated disc is the development of the cauda equina syndrome. This results when a very large fragment of disc material is ruptured into the spinal canal in the area where the nerves that control the bowels and bladder travel before they leave the spine. Pressure on these nerves can cause permanent damage to them. If this occurs, you may lose the ability to control your bowels and bladder. This is a serious problem. Fortunately, it is also rare. If your doctor suspects this is occurring, he will recommend surgery immediately to try to remove the pressure from the nerves.
During Surgery
Many complications can occur during surgery. There is always the risk of a complication due to the anesthesia used during any type of surgery. Complications that are possible during the removal of a herniated disc include:
Nerve Injury
Removing a herniated disc requires working around the nerves of the spine. During the operation, these nerves may be injured. If this occurs, you may have permanent damage to the nerve involved. This may cause permanent numbness, weakness or pain in the area where the nerve travels in the leg.Dural Tear
A watertight sack of tissue called the dura mater covers the spinal cord and the spinal nerves. A tear in this covering can occur during surgery. It is not uncommon to have a dural tear during any type of spine surgery. If this is noticed at the time of surgery, it is simply repaired and usually heals uneventfully. If it is not recognized, the tear may not heal. It may continue to leak spinal fluid. This can cause problems later. A spinal headache can result from the spinal fluid leak. A leak can also increase the risk of infection of the spinal fluid - called spinal meningitis. If the dural leak does not seal itself off fairly quickly on its own, you may need a second operation to repair the tear in the dura.After Surgery
Some complications do not show up until after surgery; some show up fairly quickly; some may take months to become evident. These include:
Infection
Any surgical operation has a small risk of infection, and operations on the spine are no different. Infection can occur in the skin incision, inside the disc, or in the spinal canal around the nerves. If an infection occurs that involves only the skin incision, you may only need antibiotics. If the infection involves the spinal canal or the disc area, you may require a second operation to drain the infection. Antibiotics will also be required after the second operation.
Re-herniation
There is always the chance (about 10-15 percent) that the same disc may herniate again. It is most likely to occur in the first six weeks after surgery, but it can occur anytime. You might need a second operation if this occurs.
Persistent Pain
Let's face it; sometimes these operations do not work. You may continue to experience pain for many reasons. Sometimes, the nerves are actually damaged by the pressure from the disc herniation and may not recover completely. You may also develop scar tissue around the nerves weeks after the operation that causes pain similar to what you had before the operation. Your pain may also be from other problems in the back that have not been corrected by removing the herniated disc.
Degenerative Disc Disease
Any injury to a disc can lead to degeneration of the spinal segment that is involved. A disc that has been operated on - and a portion removed - has definitely been injured. The development of additional back problems in the area where a disc has been removed is not certain, but there is an increased chance. This situation may require a second operation if the pain from the degenerative process becomes severe. This usually takes several years to develop.
Rehabilitation
After surgery, your doctor will probably suggest that you see a physical therapist before you start an exercise routine. Exercise is vital to recovery and to maintaining a healthy spine. Consider it part of long-term health management and risk reduction. Regular exercise is the most basic way to combat back problems. You need to make sure the exercises you choose are effective and safe for your particular case.
Why exercise? Scientific studies have shown that people who exercise regularly have far fewer problems with their back. It helps strengthen the muscles in your back that correspond with your spine. It can reduce your risk of falls and injuries. It can strengthen your abdomen (your belly), arms, and legs, which reduces back strain. Stretching reduces risk of muscle spasms. In addition, weight bearing exercises help prevent loss of bone mass caused by osteoporosis, reducing your risk of compression fractures. Aerobic exercise, the type that gets your heart pumping and pulse rate up, has been shown to be a good pain reliever as well. The natural chemicals of the body that combat pain - called endorphins - are released during exercise and actually reduce your pain.
For more information about spinal rehabilitation review the following document, entitled:
Copyright © 2003 DePuy Acromed.
