WATCHMAN Device Reduces Stroke Risk

AFib Patient No Longer Needs Blood Thinners
In 2014, while attending a church event with his wife, Jim Fulton suddenly lost vision in his right eye.
“It was really rather dramatic,” the 74-year-old St. Michaels resident recalls. “Like all of a sudden it greyed out. I actually tried to look around it. It was like somebody had dropped a curtain in front of me.”
After examining Fulton, doctors shared he had a mini stroke or transient ischemic attack (TIA) – a temporary blockage of blood flow to the brain. They traced the TIA back to atrial fibrillation (AFib), a common condition where the heart beats at an irregular, often rapid pace. AFib is a significant risk factor for stroke.
“I was asymptomatic in that I never really felt anything,” Fulton says. “I’m probably in AFib most of the time now, and I don’t notice it.”
Initially, doctors put Fulton on an anti-coagulant medicine to reduce his risk of stroke. But in 2017, Fulton was diagnosed with chronic lymphocytic leukemia, and one of the medications he took to treat the disease led to a subdural hematoma or brain bleed.
Hesitant to take anti-coagulants again but eager to prevent a stroke, Fulton turned to his cardiologist, Benjamin Remo, MD, for guidance. Dr. Remo, a physician with UM Shore Regional Health in Easton, suggested Fulton see the medical director of the University of Maryland atrial fibrillation program, to determine if Fulton could be a candidate for the WATCHMAN device.
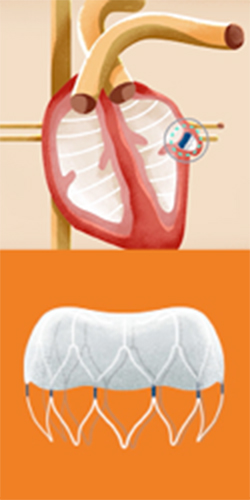
The WATCHMAN device is an FDA-approved alternative for patients who cannot tolerate long-term anticoagulation. The metal mesh device, which is about the size of a quarter, blocks the opening of the heart’s left atrial appendage to prevent blood clot formation there.
Fulton was indeed a good candidate for the device, and in October 2017, the medical director and his and team performed the procedure. He implanted the device through a catheter inserted in Fulton’s femoral vein.
Then, he guided the device into Fulton’s heart and into his left atrial appendage.
“It looks like a little metal jellyfish,” says Fulton of the WATCHMAN.
The procedure was a success, and that “jellyfish” is why Fulton is now anti-coagulant free.
“That was a big relief,” Fulton says. “If I had to take an anti-coagulant, I was putting myself at greater risk for more bleeding. The Catch-22 was that I couldn’t stop taking the anti-coagulant, but I had to stop taking the anti-coagulant. This was the way out of it.”
“While some cases of atrial fibrillation can be treated with medications and lifestyle modifications, some patients may have more difficulty controlling stroke risk or symptoms,” the director says. “These patients, like Mr. Fulton, may benefit more from procedures like the WATCHMAN to control the risk of stroke when blood thinners are not an option. Other patients with more symptoms of Afib benefit more from procedures called ablation to control their symptoms.”
“At the University of Maryland Medical Center, we began implanting the (WATCHMAN) device in 2016,” the director says. “Since then, many patients who received the device are completely off of anti-coagulant medications and are able to have peace of mind regarding their stroke risk.”
Less than a month after the WATCHMAN was implanted, Fulton says he returned to activities he enjoys, including hunting.
“I was able to engage in a strenuous outdoor activity in the cold,” he says. “The recovery period was minimal at most.”
The device also allows him and his wife, Terry, to focus on his other health issues without worrying about stroke.
“My stroke risk is no more than it would be for the normal population, and my oncologist was delighted because it frees up therapeutic alternatives for her in the event that the drugs I’m taking for cancer stop working,” he says.
Fulton says he’s thankful to the University of Maryland Medical System doctors and nurses for providing quality, continuous care from Easton to Baltimore.
“It was great,” Fulton says. “I can’t say enough good things about the doctors and the nursing staff there.”
