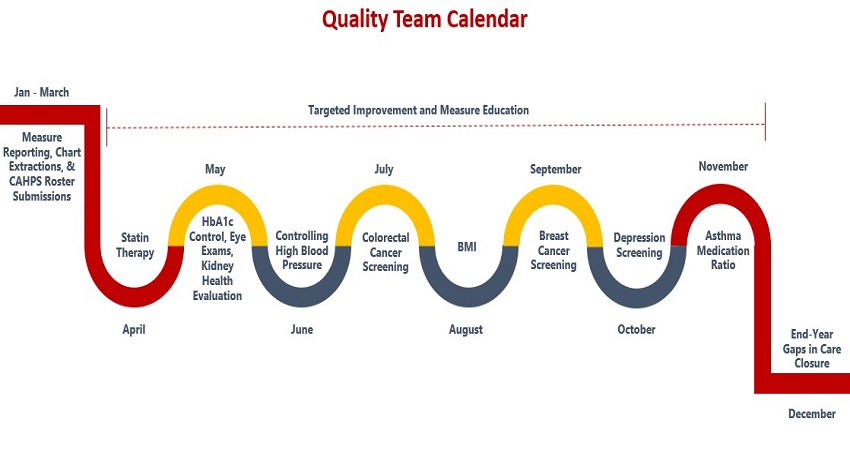
Quality and Value-Based Care
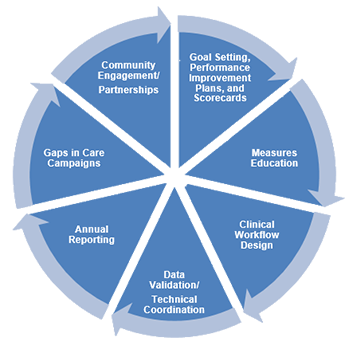
Quality, as it pertains to value-based care, requires strong multidisciplinary expertise.
Our Quality Team includes professionals with clinical, operational, technical and program policy backgrounds supporting the six domains of healthcare quality in your practice: Safe, Effective, Efficient, Timely, Equitable, and Patient-Centered.
Our Purpose
- We identify best-practice workflows that can transform quality of care delivery, meet or exceed program targets, and evolve workflows to support practice efficiency.
- We implement changes while balancing resources and provider and support staff time, and identify sustainable solutions.
- Our team of experts leverages tools and materials to engage in continuous quality improvement while prioritizing relationship-building by engaging directly with practice quality leads – clinical, operational, technical and support staff.
- We collaborate with multidisciplinary experts across the care continuum to support a comprehensive approach to quality.
What We Do
- Provide education including measure specifications, technical requirements, clinical workflow reengineering, practice workflow and EHR process, and workflow re-engineering
- Guide practices in targeted improvement and implementation of best practices (inclusive of regulatory requirements and industry standards)
- Provide monthly metric-level performance reviews and analytical insight
- Provide technical guidance for third-party vendors related to measure specifications, chart extractions, and Consumer Assessment of Healthcare Providers and Systems (CAHPS) rosters
- Cross-team collaboration with Care Management, Finance, Informatics, Data Integration, Practice Transformation and Risk Adjustment